Actuarial-Grade Intelligence
Powered by the Acumen Platform
The Acumen platform is your single source of truth - curated from messy, multi-source data, enriched with deep healthcare domain logic, and engineered for precision.
What Acumen Delivers
No dashboards. No disruption. No integration headaches.
Contract with Confidence
Benchmark, price, and structure value-based arrangements with actuarial-grade data. Unify messy claims into a clean foundation you can trust - then stratify risk, assess historicals, and set terms that hold up.
Monitor What Matters
Track cost, utilization, and quality - aligned to your unique contracts. Measure contract performance in real time, not just at reconciliation, with data mapped to your exact inclusion/exclusion logic.
Stay Ahead of Financial Risk
Spot issues early and act before costs spike. Project total cost of care, identify rising-risk members, and intervene early using predictive and IBNR models.
Empower Partners
Equip partners with data they'll actually use. Deliver simple, actionable reports - no black box, no dashboards - so providers can improve care and hit targets.
End the Integration Firefights
Skip the ETL chaos - Acumen delivers data that's ready to go. We ingest, validate, normalize, and enrich multi-source data so your team can focus on insights, not cleanup.
Grow Smarter
Surface opportunity, win referrals, and scale high-performing care. Use performance data and benchmarking to fuel growth - by proving impact and identifying where to expand.
Available Data Models
Modular and purpose-built to power smarter decisions in value-based care, Acumen delivers ready-to-use data - no dashboards, no black box, no integration headaches.
Membership
A unified view of your population. Know who your members are, where they've been, and how they're attributed.
Claims Data Categorization (CDC)
Normalize and enrich claims data into service types, clinical groupings, and cost categories - so you can analyze cost, utilization, and care patterns instantly.
Contract Performance (CP)
Measure performance against each contract's terms. Track cost of care, set reserves, and guide financial strategy year-round.
Dynamic Benchmarking (DB)
Compare cost and utilization performance to peer benchmarks, tailored to your population. Find strengths to build on and gaps to fix - before they impact results.
Episode Benchmark (EB)
Benchmark episode performance against market peers. Spot outliers, reduce unnecessary services, and align specialty care to best practice.
Episode Grouper (EG)
Structure claims into episodes of care, from surgery prep to recovery. Evaluate performance by specialty, optimize referrals, and negotiate smarter specialty contracts.
Incurred But Not Reported Estimates (IBNR)
Estimate total cost of care - even before all claims are in. Supports timely reserving, forecasting, and risk adjustment calculations.
Medical Event Prediction (MEP)
Predict which members will experience high-cost events - like admissions or joint replacements - and trigger interventions that prevent escalation.
Member Risk Stratification (MRS)
Stratify your population by predicted cost, condition, and avoidable utilization. Prioritize outreach where it makes the biggest difference.
Risk Adjustment (RA)
Identify missed or undocumented HCCs using a blend of claims evidence, EHR data, and predictive modeling. Supports CMS-HCC and HHS-HCC, including multiple model years.
Compatible By Design
Acumen supports external models like Tuva's out of the box - so if your team's already using it, we'll meet you where you are. We'll integrate Tuva's schema and deliver alongside Acumen.
How It Works
Frictionless integration that transforms your raw data into actuarial-grade insights without disrupting your existing workflow.
Simple. Powerful. Direct.
Accorded connects directly to your existing data warehouse, applying actuarial-grade transformations to deliver clean, structured tables ready for immediate use in your business applications.
1. We connect to your data
2. Acumen curates your data using actuarial-grade logic and modern data engineering
3. Insights continuously drop into your warehouse - clean, enriched, and ready to use
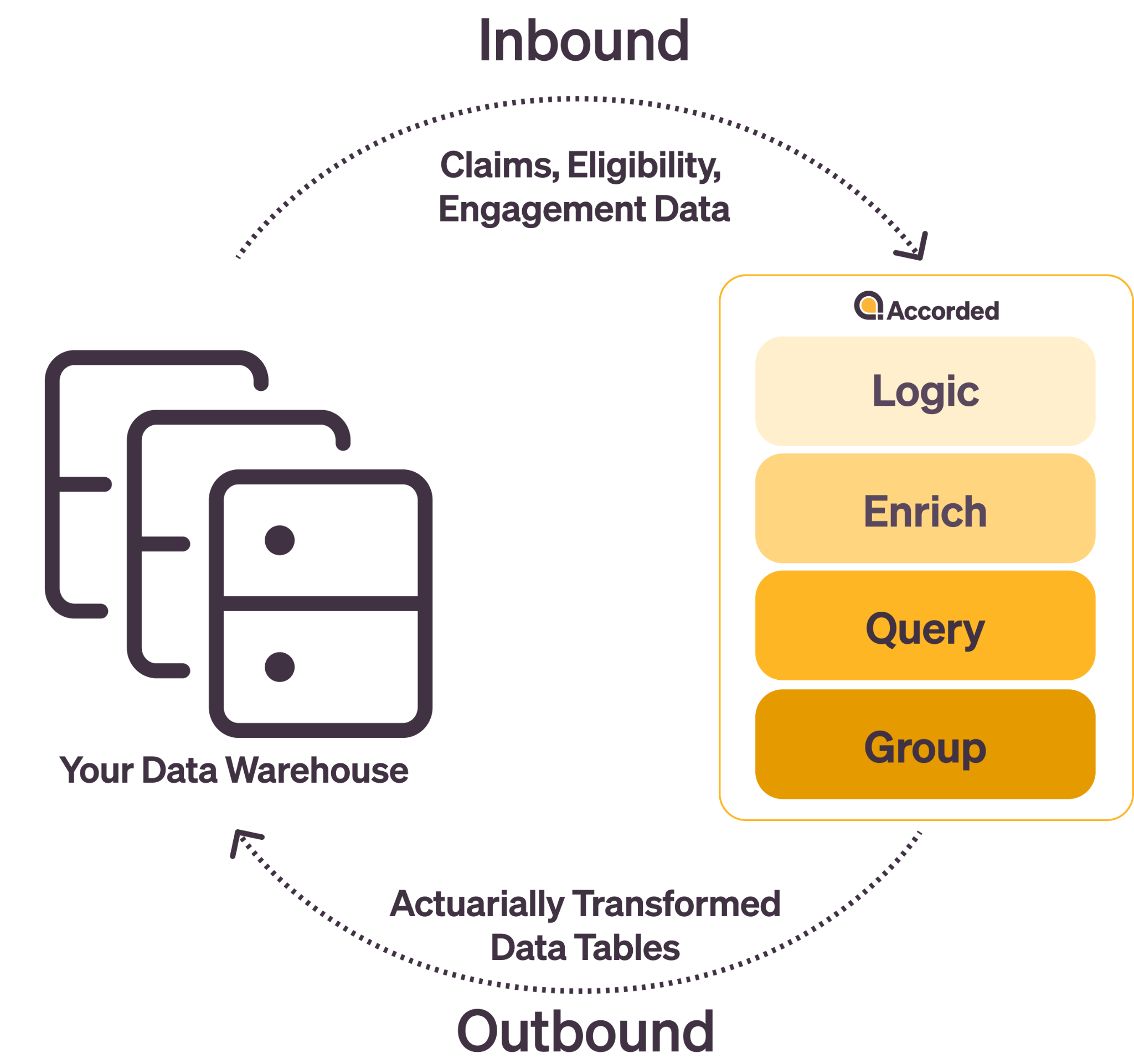
No dashboards to learn. No workflow disruption. No data engineering headaches. Just clean, contract-aligned data delivered where you need it.
Client Success Story

Zachery Chen
SVP & Head of Finance

How Gather Health transformed their risk-based contract performance with Acumen
What were the pain points that you were trying to solve for?
- Lean analytics team with bandwidth constraints.
- Lack of in-house actuarial subject matter expertise for data contextualization.
- Need for rapid time-to-value for new risk-based contracts, requiring immediate performance insights.
Why did you choose Accorded / what were you looking for in a partner?
- Actuarial contextualization of the data was essential to ensure data accuracy and completeness.
- Transparency in data transformation processes was a critical requirement.
- The solution needed to augment, not replace, our existing in-house capabilities.
- As a risk-bearing entity, medical economics and actuarial expertise are considered core competencies, and our vendor of choice needed to support this.
- Accorded's focused approach allowed us to address immediate needs without purchasing an extensive, potentially unnecessary suite of services.
How has your journey with Accorded been so far?
- We partnered with Accorded to analyze the medical and financial performance of our at-risk payer contracts. Accorded's Acumen product seamlessly integrates data across our EMR and 30+ distinct payer files to deliver enriched data models that directly integrate with our data warehouse.
- Accorded is helping us effectively assess our risk pool and our performance based on our contract metrics.
- With the support of the Accorded team, we continue to identify key trends across our patient population and our provider network to make informed and proactive decisions.
Gather Health's mission is to improve lives and communities for older adults by championing socially-supported and holistic primary care as a neighborhood interest
Why It Pays Off
Transform how your organization manages risk. Move from reactive data firefighting to proactive strategy execution with measurable impact on your bottom line.
- Grow revenue with smarter contracts
- Contain costs before they escalate
- Prove performance - and earn trust
- No more firefighting data integration issues
- Guide action that changes outcomes
- Simplify oversight at scale